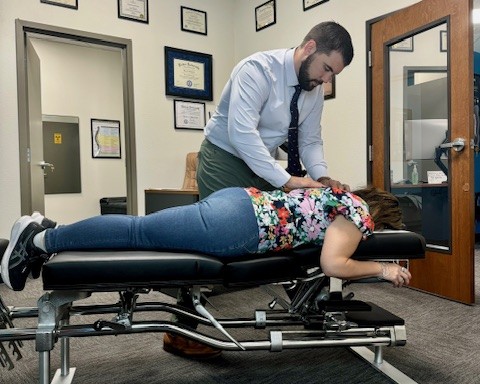
If you’ve been told you have a herniated disc, you’re probably feeling overwhelmed, worried, and maybe even a little scared about what comes next. It’s completely understandable. A herniated disc diagnosis can sound serious, and the pain that often comes with it can interfere with your daily life in frustrating ways. But here’s the good news: most herniated discs improve with conservative, non-surgical care, and understanding your condition is the first step toward feeling better. Here at Castle Hills Chiropractic in Castle Hills, TX, we work with patients every day who are navigating herniated disc recovery, and we’re here to help you understand what’s happening in your spine, what your treatment options look like, and how to move forward with confidence.
What is a herniated disc? A herniated disc occurs when the soft, gel-like center of a spinal disc pushes through a tear or weakness in the tough outer layer. This can irritate nearby nerves and cause pain, numbness, tingling, or weakness in the back, neck, arms, or legs, depending on where the herniation occurs.
Table of Contents
- Understanding Herniated Discs: What’s Really Happening
- Common Causes and Risk Factors
- Signs and Symptoms to Watch For
- The Diagnosis Process: What to Expect
- How Chiropractic Care Fits Into Herniated Disc Treatment
- Treatment Options: Conservative Care First
- Recovery Timeline and What Affects It
- Practical Tips for Daily Living with a Herniated Disc
- When to See a Chiropractor
- Treatment Approaches Comparison
- Myths vs. Facts About Herniated Discs
- Final Thoughts
Understanding Herniated Discs: What’s Really Happening
Your spine is made up of vertebrae stacked on top of one another, with intervertebral discs cushioning between them. These discs act like shock absorbers, allowing your spine to bend, twist, and handle the forces of everyday movement. Each disc has two main parts: a tough, fibrous outer ring called the annulus fibrosus, and a soft, jelly-like center called the nucleus pulposus.
When we talk about herniated discs, we’re describing what happens when that inner gel-like material pushes through a crack or tear in the outer ring. You might also hear this called a “slipped disc” or “ruptured disc,” though technically the disc doesn’t slip out of place. Instead, the inner material bulges or leaks out, which can press on nearby spinal nerves or the spinal cord itself.
Here in Castle Hills, TX, many patients come to Castle Hills Chiropractic wondering if their herniated disc means they’ll need surgery or if they’ll be dealing with pain forever. The reality is that most herniated discs respond well to conservative care. The body has a remarkable ability to heal, and the herniated material can sometimes shrink over time as inflammation decreases and the body reabsorbs it.
Herniated discs can happen anywhere along the spine, but they’re most common in two areas: the lower back (lumbar spine) and the neck (cervical spine). Lumbar herniations often cause sciatica, which is pain that radiates down the leg. Cervical herniations can cause pain, numbness, or tingling that travels into the shoulder, arm, and hand.
Common Causes and Risk Factors
Understanding what causes herniated discs can help you make sense of your diagnosis and take steps to prevent future problems. While some herniations happen due to a specific injury or accident, many develop gradually over time due to wear and tear on the spine.
Age-related degeneration is one of the most common factors. As we get older, our discs naturally lose some of their water content, making them less flexible and more prone to tearing. This process, called disc degeneration, is a normal part of aging, but it increases the risk of herniation.
Repetitive strain and poor mechanics also play a significant role. Jobs or activities that involve frequent bending, lifting, twisting, or sitting for long periods can put extra stress on your spinal discs. When these movements are done with poor posture or improper technique, the risk goes up even more.
Sudden trauma or injury can cause a disc to herniate immediately. This might happen during a car accident, a fall, or while lifting something heavy with improper form. However, it’s worth noting that even when a herniation seems to happen suddenly, the disc may have already been weakened by years of gradual wear and tear.
Lifestyle factors that increase your risk include being overweight (which puts extra pressure on the discs in your lower back), smoking (which reduces oxygen supply to spinal tissues and accelerates degeneration), and leading a sedentary lifestyle (which weakens the muscles that support your spine).
Genetics can also play a role. Some people are simply more prone to disc problems due to inherited traits that affect the strength and structure of their spinal tissues.
Signs and Symptoms to Watch For
The symptoms of herniated discs vary widely depending on the location and severity of the herniation, and whether it’s pressing on a nerve. Some people have a herniated disc without even knowing it, while others experience significant pain and disability.
If the herniation is in your lower back (lumbar spine), you might experience sharp or aching pain in the lower back itself, but more commonly, you’ll feel pain that radiates down one leg. This is because the herniated disc material presses on the sciatic nerve, causing what we call sciatica. You might feel shooting pain, burning, tingling, or numbness that travels from your buttock down through your thigh, calf, and sometimes all the way to your foot. Weakness in the leg or foot can also occur, making it difficult to walk on your toes or heels.
If the herniation is in your neck (cervical spine), symptoms typically affect your shoulder, arm, and hand. You might experience neck pain, but the more bothersome symptoms are often the radiating pain, tingling, numbness, or weakness that travels down one arm. Some patients describe it as an electric shock sensation or a burning feeling.
In some cases, herniated discs cause symptoms without much back or neck pain at all. The radiating symptoms are the primary complaint, which can sometimes make diagnosis tricky if patients don’t connect their arm or leg symptoms to a spinal problem.
Symptoms often worsen with certain movements or positions. Sitting, bending forward, coughing, or sneezing can increase the pressure inside the disc and worsen symptoms. Many patients find relief when standing, walking, or lying down.
The Diagnosis Process: What to Expect
Getting an accurate diagnosis is crucial for developing an effective treatment plan. When you visit Castle Hills Chiropractic with concerns about a possible herniated disc, we start with a thorough consultation and examination.
During your consultation, we’ll discuss your symptoms in detail: when they started, what makes them better or worse, and how they’re affecting your daily life. We’ll also review your medical history and any previous spine problems or injuries.
The physical examination includes several components. We’ll assess your posture, range of motion, and movement patterns. We’ll perform orthopedic and neurological tests to check your reflexes, muscle strength, and sensation in your arms or legs. Specific tests help us determine if nerve compression is present and which nerve root might be affected.
Imaging studies are often helpful but not always necessary, especially in the early stages. Many herniated discs can be diagnosed clinically based on your symptoms and examination findings. If imaging is needed, an MRI is the gold standard because it clearly shows the soft tissues, including the discs and nerves. X-rays don’t show herniated discs themselves but can rule out other problems like fractures or significant arthritis. CT scans are sometimes used when MRI isn’t available or appropriate.
It’s important to understand that finding a herniated disc on an MRI doesn’t automatically mean it’s the cause of your pain. Research has shown that many people without any back pain have herniated discs visible on imaging. This is why correlating your symptoms with examination findings is so important.
How Chiropractic Care Fits Into Herniated Disc Treatment
Chiropractic care offers a conservative, non-surgical approach to managing herniated discs. At Castle Hills Chiropractic, our goal is to reduce pain, improve function, and support your body’s natural healing process.
We use gentle, specific chiropractic adjustments tailored to your condition. For herniated discs, we typically avoid techniques that involve twisting or rotation in the area of herniation. Instead, we use methods like flexion-distraction, which involves gentle stretching and decompression of the spine. This technique can help reduce pressure on the affected disc and nerve, decrease inflammation, and promote healing.
Our approach is always individualized. We consider the location and severity of your herniation, your symptoms, and your overall health. Some patients respond beautifully to chiropractic care alone, while others benefit from a combination approach that might include therapeutic exercises, soft tissue work, and lifestyle modifications.
Chiropractic care for herniated discs focuses on restoring proper spinal alignment and movement, which can take pressure off the affected disc and nerve. We also work on improving the function of surrounding joints and muscles, which helps support the injured area during healing.
Evidence suggests that chiropractic care can be effective for many patients with herniated discs, particularly those with lumbar disc herniations causing sciatica. A 2014 study published in the Journal of Manipulative and Physiological Therapeutics found that chiropractic care was associated with significant improvements in pain and disability for patients with lumbar disc herniation.
Treatment Options: Conservative Care First
The good news about herniated discs is that research consistently shows that conservative treatment is effective for the vast majority of patients. Surgery is rarely the first option and is typically reserved for cases where conservative care hasn’t helped or when there are serious neurological symptoms.
Chiropractic care, as discussed above, is a cornerstone of conservative treatment. Gentle adjustments, spinal decompression, and therapeutic exercises can all play important roles in your recovery.
Physical therapy often complements chiropractic care. A physical therapist can teach you specific exercises to strengthen your core muscles, improve flexibility, and support your spine. These exercises help prevent future problems and speed recovery.
Modified activity and rest are important in the early stages. This doesn’t mean complete bed rest, which is generally not recommended for more than a day or two. Instead, it means avoiding activities that worsen your symptoms while staying as active as possible within your pain limits. Movement promotes healing by bringing nutrients to the disc and removing waste products.
Pain management might include over-the-counter medications like NSAIDs (non-steroidal anti-inflammatory drugs) to reduce inflammation and pain. Some patients benefit from ice or heat therapy. Always consult with your healthcare provider about appropriate pain management strategies for your situation.
Epidural steroid injections are sometimes used when pain is severe and not responding to other conservative measures. These injections deliver anti-inflammatory medication directly to the area around the affected nerve and can provide temporary relief that allows you to participate more effectively in physical rehabilitation.
Surgery is considered when conservative treatment hasn’t provided adequate relief after several weeks to months, or when there are red flag symptoms like severe or progressive weakness, loss of bladder or bowel control, or severe pain that significantly impairs quality of life. The most common surgical procedure for herniated discs is a discectomy, where the herniated portion of the disc is removed.
Recovery Timeline and What Affects It
One of the most common questions patients ask is, “How long will it take to get better?” The honest answer is that it varies considerably from person to person, but understanding the general timeline can help set realistic expectations.
For most people with herniated discs, significant improvement occurs within 4 to 6 weeks of starting conservative treatment. Many patients notice their symptoms beginning to ease within the first couple of weeks. However, complete resolution of symptoms can take several months, and some people experience occasional flare-ups even after the initial recovery.
Several factors influence your recovery timeline. The severity of the herniation matters. Smaller bulges or protrusions often heal faster than large extrusions where disc material has broken through completely. Whether a nerve is compressed also affects recovery. Nerve symptoms like numbness and weakness often take longer to resolve than pain alone.
Your overall health plays a significant role. People who are physically fit, at a healthy weight, and don’t smoke tend to heal faster. Age can be a factor, as younger patients sometimes heal more quickly, though older patients can still have excellent outcomes with appropriate care.
Compliance with treatment is crucial. Patients who consistently follow through with their chiropractic appointments, do their prescribed exercises at home, and make recommended lifestyle modifications typically recover faster and more completely than those who don’t.
Psychological factors also influence recovery. Research has shown that stress, anxiety, fear of movement, and catastrophic thinking about pain can all slow recovery and increase the risk of chronic pain. Maintaining a positive but realistic outlook, staying engaged in activities you enjoy (within your limitations), and managing stress can all support healing.
Practical Tips for Daily Living with a Herniated Disc
While you’re recovering from a herniated disc, there are many things you can do at home to support healing and manage your symptoms. These strategies are safe, effective, and align with what we recommend at Castle Hills Chiropractic in Castle Hills, TX.
Maintain proper posture throughout the day. When sitting, use a chair with good lumbar support, keep your feet flat on the floor, and avoid slouching. If you work at a desk, make sure your computer screen is at eye level so you’re not constantly looking down, which can strain your neck if you have a cervical herniation.
Modify your sleeping position to minimize stress on your spine. If you have a lumbar herniation, sleeping on your back with a pillow under your knees or on your side with a pillow between your knees can help. For cervical herniations, use a pillow that keeps your neck in a neutral position, neither too high nor too flat.
Use proper lifting technique always, but especially during recovery. Bend at your knees, not your waist. Keep the object close to your body. Avoid twisting while lifting. Better yet, avoid heavy lifting entirely until your symptoms have significantly improved.
Stay active within your limits. Walking is often well-tolerated and beneficial. Start with short walks and gradually increase distance as tolerated. Swimming or water aerobics can be excellent because the water supports your body weight, reducing stress on your spine.
Apply ice or heat as recommended by your chiropractor. Ice can help reduce inflammation in the early stages, while heat can relax tight muscles and improve circulation later in recovery. Never apply ice or heat directly to skin; always use a barrier like a towel.
Practice gentle stretching and movement to maintain flexibility and prevent stiffness. Your chiropractor can show you specific stretches that are safe and beneficial for your particular herniation. Avoid any stretches or movements that increase your pain or radiating symptoms.
Manage stress through relaxation techniques, deep breathing, meditation, or activities you enjoy. Chronic stress can increase muscle tension and pain perception, slowing your recovery.
Maintain a healthy weight. Extra body weight puts additional stress on your spinal discs, particularly in the lower back. If weight is an issue, work toward gradual, sustainable weight loss through healthy eating and appropriate exercise.
When to See a Chiropractor
If you’re experiencing back pain with or without leg pain, or neck pain with or without arm symptoms, it’s worth getting evaluated by a chiropractor. Early assessment and treatment often lead to better outcomes and can prevent a minor problem from becoming a major one.
Specific situations where you should seek care include: pain that radiates down your arm or leg, especially if it’s accompanied by numbness or tingling; pain that’s worse when sitting, bending, coughing, or sneezing; back or neck pain that persists for more than a few days or keeps returning; pain that interferes with your work, sleep, or daily activities; or symptoms that developed after an injury or accident.
The duration and severity of your symptoms matter. Acute back pain that’s mild to moderate might improve on its own with rest and over-the-counter pain relief, but if symptoms persist beyond a week or two, professional evaluation is wise. Severe pain from the start warrants earlier assessment.
There are also red flag symptoms that require immediate medical attention. Seek emergency care if you experience: loss of bladder or bowel control (difficulty urinating or having bowel movements, or loss of sensation in your groin or rectal area); progressive weakness in your legs or feet, especially if it’s affecting your ability to walk; numbness or tingling in both legs simultaneously; severe pain that’s not relieved by any position or medication; or symptoms accompanied by fever, unexplained weight loss, or a history of cancer.
Here at Castle Hills Chiropractic, we’re trained to recognize these warning signs. If we identify symptoms that require medical referral or emergency care, we’ll make sure you get to the right provider immediately. Your safety is always our top priority.
Treatment Approaches Comparison
| Treatment Approach | Primary Goal | Typical Timeline | Best Suited For |
|---|---|---|---|
| Chiropractic Care | Restore spinal alignment, reduce nerve pressure, promote natural healing | 4-12 weeks of regular care | Most herniated disc patients, especially with mechanical pain |
| Physical Therapy | Strengthen supporting muscles, improve flexibility and function | 6-12 weeks of exercises and manual therapy | Patients needing rehabilitation and core strengthening |
| Pain Medication | Reduce inflammation and manage pain symptoms | Short-term use, days to weeks | Acute phase when pain limits function and participation in therapy |
| Epidural Injections | Deliver anti-inflammatory medication directly to affected area | Effects last weeks to months | Moderate to severe nerve pain not responding to other conservative care |
| Surgery | Remove herniated disc material compressing the nerve | Recovery takes 6 weeks to 6 months | Severe cases with red flag symptoms or failed conservative treatment |
Myths vs. Facts About Herniated Discs
Myth: A herniated disc always requires surgery
Fact: The vast majority of herniated discs heal with conservative treatment. Research indicates that 80-90% of patients improve without surgery. Surgery is typically reserved for cases with severe neurological symptoms or when conservative care hasn’t provided adequate relief after several months.
Myth: If you have a herniated disc, you should avoid all physical activity
Fact: While you should avoid activities that worsen your symptoms, staying active within your limits is actually important for recovery. Movement helps bring nutrients to the disc and surrounding tissues. Complete bed rest for more than a day or two can actually slow healing and lead to muscle weakness and stiffness.
Myth: Once a disc herniates, the damage is permanent
Fact: The body has a remarkable ability to heal herniated discs. Research has shown that herniated disc material can shrink or even completely resorb over time. While the disc may not return to its original state, many people make complete functional recoveries and return to all their normal activities.
Myth: Chiropractic adjustments will make a herniated disc worse
Fact: When performed by a trained chiropractor who understands herniated disc conditions, chiropractic care is generally safe and can be very effective. We use gentle, specific techniques appropriate for your condition. We avoid aggressive manipulation in the area of acute herniation and instead focus on techniques that decompress and support healing.
Myth: You can feel your disc “slip out of place”
Fact: Discs don’t actually slip in and out of position. They’re firmly attached between the vertebrae. What you might feel when you have sudden back pain is a muscle spasm, joint irritation, or the beginning of a herniation, but the disc itself isn’t slipping around. The term “slipped disc” is a misleading nickname for herniation.
Myth: Herniated discs only happen to older people
Fact: While disc degeneration is more common as we age, herniated discs can occur at any age. Young people can herniate discs due to injury, poor lifting mechanics, or repetitive strain. We see patients of all ages at Castle Hills Chiropractic with herniated disc issues.
Final Thoughts
Dealing with a herniated disc can be challenging, but it’s important to remember that you have options and that most people get better with the right care and support. At Castle Hills Chiropractic here in Castle Hills, TX, we’re committed to helping our patients navigate herniated disc recovery with evidence-based, conservative care that respects your body’s natural healing abilities.
Whether you’re just starting to experience symptoms or you’ve been dealing with disc problems for a while, we encourage you to reach out for an evaluation. Understanding your specific situation is the first step toward feeling better, and we’re here to provide that clarity and develop a treatment plan that makes sense for you.
Remember, healing takes time, but with patience, consistency, and the right guidance, you can absolutely improve and get back to the activities you love. We see it happen every day in our practice, and we’d be honored to be part of your recovery journey.
Frequently Asked Questions
Can a herniated disc heal on its own without treatment?
Yes, many herniated discs do improve on their own over time as inflammation decreases and the body’s natural healing processes take effect. However, conservative treatment like chiropractic care, physical therapy, and appropriate activity modification typically speeds recovery and provides symptom relief during the healing process.
How long does it take for a herniated disc to heal?
Most people see significant improvement within 4 to 6 weeks of starting treatment, though complete resolution can take several months. Recovery time varies based on the severity of herniation, your overall health, and how consistently you follow treatment recommendations.
Will I need an MRI to diagnose a herniated disc?
Not always. Many herniated discs can be diagnosed based on your symptoms and physical examination findings. An MRI is typically ordered if symptoms don’t improve with initial treatment, if neurological symptoms are severe, or if surgery is being considered. Your chiropractor will help determine if imaging is necessary in your case.
Can I exercise with a herniated disc?
Yes, but you should choose exercises carefully and avoid activities that increase your pain or radiating symptoms. Walking, swimming, and gentle stretching are often well-tolerated. Your chiropractor can recommend specific exercises that are safe and beneficial for your particular herniation.
Is it safe to get adjusted by a chiropractor if I have a herniated disc?
Yes, chiropractic care can be safe and effective for herniated discs when performed by a qualified chiropractor. We use gentle, specific techniques appropriate for your condition, avoiding aggressive manipulation in areas of acute herniation. We always perform a thorough examination first and tailor our approach to your specific needs.
What’s the difference between a herniated disc and a bulging disc?
A bulging disc occurs when the outer layer of the disc weakens and the disc material expands beyond its normal boundary, but the outer layer remains intact. A herniated disc involves a tear in the outer layer through which the inner gel-like material leaks out. Herniated discs are more likely to cause nerve compression and radiating pain, though both conditions can be treated conservatively.
TL;DR – Key Takeaways
- Herniated discs occur when the inner disc material pushes through the outer layer, potentially pressing on nerves and causing pain, numbness, or weakness in the back, neck, arms, or legs.
- Most herniated discs (80-90%) improve with conservative treatment including chiropractic care, physical therapy, and lifestyle modifications – surgery is rarely the first option.
- Recovery typically takes 4-6 weeks for significant improvement, though complete healing may take several months depending on severity and individual factors.
- Safe, effective self-care strategies include maintaining proper posture, staying active within your limits, using appropriate sleeping positions, and practicing gentle stretching as recommended by your chiropractor.
- Seek immediate medical attention for red flag symptoms including loss of bladder/bowel control, progressive weakness, or severe unrelenting pain, but for most herniated disc symptoms, conservative chiropractic care is an appropriate first step.